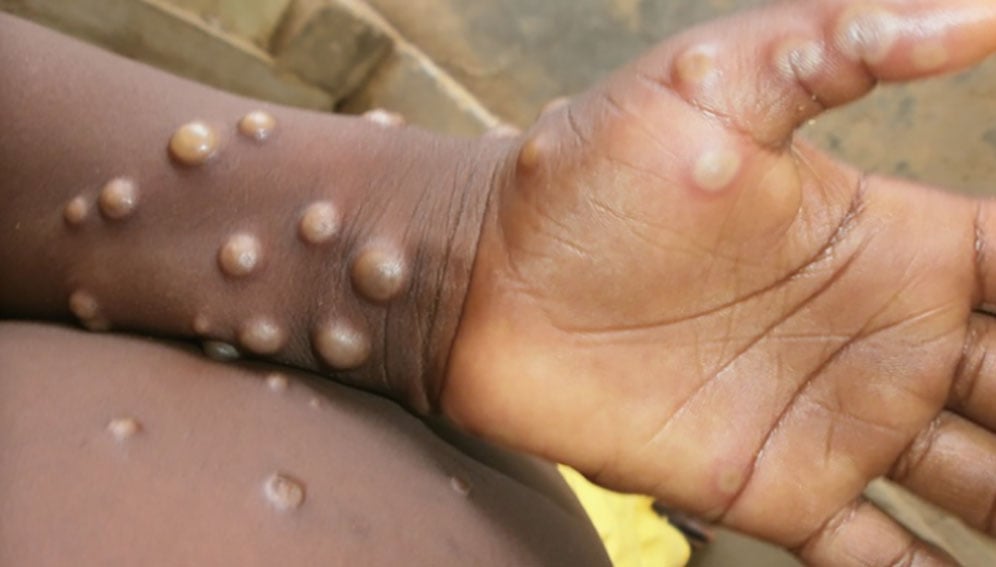
[LAGOS, SciDev.Net] New evidence suggests that mpox may be circulating quietly among healthy Nigerians, with some infections occurring without the symptoms that typically trigger detection by health authorities.
The evidence comes from a collaborative study by Nigeria’s Institute of Human Virology, the University of Cambridge, in the UK, and others, published in Nature Communications.
While the researchers stress that this does not indicate a widespread hidden epidemic, they warn that such silent exposure could be bypassing Nigeria’s surveillance systems.
“What we are seeing is evidence that mpox exposure doesn’t always look like the textbook description,” Adam Abdullahi, the study’s lead author told SciDevNet.
“In some people, particularly in settings with partial population immunity, the virus may circulate quietly, leaving immune footprints that routine clinical surveillance will miss.”
The study comes at a critical moment for Nigeria’s public health response. In 2024, the country became the first in Africa to begin an mpox vaccine rollout, largely guided by reported symptomatic cases.
But the new evidence raises questions about whether symptom-based surveillance alone is sufficient to inform vaccination strategies.
Mpox is a zoonotic disease caused by the MPXV virus, spreading through animal-to-human or close person-to-person contact. It is commonly associated with fever, swollen lymph nodes and a painful rash.
For decades, protection against mpox came indirectly through routine smallpox vaccination, which ended globally after smallpox was eradicated in 1980.
Since then, a growing proportion of the population has lacked this immunity. In Nigeria and across parts of West and Central Africa, this shift has coincided with renewed mpox transmission, including outbreaks recorded between 2022 and 2024.
Hidden exposure
To better understand how widely the virus may be circulating, the scientists analysed archived blood samples from 176 healthy Nigerian adults originally enrolled in SARS-CoV-2 vaccine studies. The samples were collected from healthcare workers in 2021 and community volunteers in 2023.
None of the participants had received mpox or smallpox vaccination in adulthood, and none were known to have been exposed to mpox.
The results showed that 14 per cent of participants had retained antibodies linked to historic smallpox vaccination, concentrated among those born before 1980—the last generation to receive childhood vaccinations. This finding reflects what scientists call a generational “immunity gap”.
However, an unexpected finding was also identified. When follow-up samples were collected from participants—typically after around nine months—about 3 per cent showed clear evidence of a new immune response, consistent with recent mpox exposure. These individuals had no recorded mpox diagnosis and did not report any related symptoms.
The researchers say this suggests mpox is spreading silently, bypassing traditional healthcare surveillance.
‘Low-level’ spread
To contextualise these findings, the team analysed over 100 mpox genomes collected across Nigeria. The data indicates that while the virus continues to circulate, its spread is constrained by residual immunity in older populations, according to the researchers.
Ravindra Gupta, a senior author on the study from the Cambridge Institute of Therapeutic Immunology and Infectious Disease, said the results point to sustained low-level transmission rather than unchecked spread.
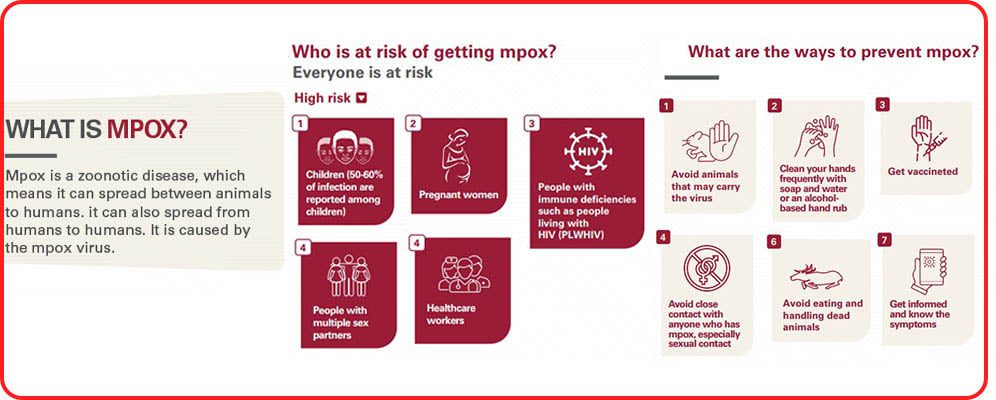
Some facts on mpox. Adapted from Africa CDC
“Mpox is not spreading unchecked in Nigeria and across the region, but neither is it absent,” he said. “Instead, it appears to circulate at low levels, shaped by the lingering effects of smallpox vaccination in older generations.”
The researchers also found no significant difference in immune responses between healthcare workers and the general population, suggesting that exposure is not limited to clinical settings.
Surveillance blind spot
Nigeria’s mpox surveillance system, like those in many African countries, relies heavily on identifying people who present at health facilities with visible symptoms.
While this approach works well for detecting obvious outbreaks, the study points to a blind spot in missing the silent circulation now being found in healthy adults.
Addressing this vulnerability would require a fundamental shift in how Nigeria tracks the virus. Experts argue that because silent transmission bypasses traditional hospital checks, a new diagnostic approach is needed.
Alash’le Abimiku, executive director of the International Research Center of Excellence of the Nigerian Institute of Human Virology, believes antibody-based surveillance could help fill this gap.
“Instead of relying solely on reported cases or symptoms, monitoring populations by testing blood samples for antibodies can reveal exposure to the virus and help us understand how it is spreading,” she said.
“This is important for guiding targeted vaccination in our settings.”
Abdullahi agrees, noting that antibody surveillance offers a way to detect exposure in people who never visit clinics.
“If we only look for obvious disease, we will miss part of the picture,” he said.
“Monitoring blood samples allows us to see transmission that does not result in clinic visits, especially in regions where health systems are already are stretched and require strengthening.”
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.